This article was written by Lisa Miller.
Hospital Assessment of SDOH Readiness
Social determinants of health (SDOH) continues to emerge as a significant healthcare trend for 2020, increasing the need for your hospital to carry out an assessment of SDOH readiness.
Healthcare providers are recognizing the significance of this issue by investing in programs focusing on areas such as housing insecurity and employment.
New research found that SDOH programs accounted for around $2.5 billion of spend. [1] That figure is expected to rise.
Value based care remains the basis for reimbursement. However, improving individual and population health outcomes, and providing high quality care while reducing healthcare costs are the goals set by healthcare systems.
The impact of SDOH on patient outcomes
 Multiple studies show that clinical outcomes are based on factors which include the medical care a patient receives, as well as a patient’s social and environmental circumstances.
Multiple studies show that clinical outcomes are based on factors which include the medical care a patient receives, as well as a patient’s social and environmental circumstances.
These social needs are known as the social determinants of heath (SDOH) and are a fundamental premise in addressing the health of patients nationwide.
“Healthy People 2020 highlights the importance of addressing the social determinants of health by including ‘Create social and physical environments that promote good health for all’ as one of the four overarching goals for the decade.” [2]
Healthcare leaders are focused on ways they can address these SDOH within their communities to:
- Increase quality outcomes.
- Decrease the hospital readmissions rate.
- Develop innovative programs to assist patients with chronic conditions.
That requires all hospitals to develop a ‘’SDOH Readiness Plan’’ by creating strategic goals and coordinating with multiple stakeholders, including hospital leadership and employees, physician practices, payers and community partners.
Furthermore, this task requires the full commitment of your hospital’s executive leadership to invest in programs designed to address the specific needs and improve the health of the patients they serve.
Here’s our advice on how to create a SDOH Readiness Plan for your hospital:
5 Steps to the SDOH Readiness Plan
Step 1: Identify the critical social needs in your community
The Patient Protection and Affordable Care Act of 2010 (ACA) requires tax-exempt hospitals to create a hospital community health needs assessment every three years.
This assessment can serve as the launch pad for developing innovative SDOH programs within your hospital community. Although this assessment is mandatory, many of the socioeconomic needs identified often present multiple challenges and barriers. Your strategic plan must therefore set realistic goals, identify financial resources and grant opportunities, and engage with community partners if it is to be successful.
“When asked about barriers to general dissemination of innovations, practices and hospitals that did not screen for social needs were significantly more likely to report a lack of financial resources, time, and incentives as major barriers” [3]
After reviewing the Community Needs Assessment, the next step is to identify which social needs to focus on that will have the greatest positive impact in your community.
We recommend the use of the Healthy People 2020 Framework in your hospital’s decision making process:
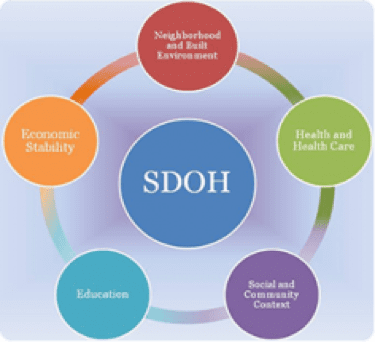
- Economic Stability (employment, food and housing insecurity, poverty).
- Education (early childhood, high school graduation, language and literacy).
- Social and Community Context (civic participation, discrimination, incarceration, social cohesion).
- Health and Healthcare (access to healthcare, transportation, health literacy).
- Neighborhood and Built Environment (access to health food, crime and violence, quality of housing, environmental conditions).
Step 2: Identify the social needs of your patient community
The second step involves the utilization of a screening tool to identify the social needs of your patients. Although many academic facilities and practices serving disadvantaged patients have established a screening process, most screen for only one or two social needs.
A 2019 study surveyed 2190 physician practices and 739 hospitals to identify whether they screened patients for five key social needs. The five key social needs associated with health outcomes included interpersonal violence, transportation needs, utility needs, housing instability and food insecurity.
The results revealed that most hospitals and physician practices do not screen for all five social needs. Only 15.6% of physician practices and 24.4% of hospitals reported screening for all 5 social needs. [3]
Only 15.6% of physician practices and 24.4% of hospitals report screening for all 5 social needs related to SDOH. Click To Tweet
“This study’s findings suggest that few US physician practices and hospitals screen patients for all 5 key social needs associated with health outcomes. Practices that serve disadvantaged patients report higher screening rates. The role of physicians and hospitals in meeting patients’ social needs is likely to increase as more take on accountability for cost under payment reform. Physicians and hospitals may need additional resources to screen for or address patients’ social needs.”
Multiple departments must be involved in the design process to implement an effective, system wide screening tool and follow up. A collaborative team approach should include representations from hospital leadership, IT, nursing, HIM, patient access, social work, dieticians, rehabilitation and so on.

Once the SDOH readiness team is established, this group must develop a customized plan based on hospital specific needs. Some examples of project initiatives include:
- Determine if your EHR infrastructure will capture SDOH data in an admission screening tool. Note: EPIC is testing a SDOH tool in their EHR. [5] If this is not electronic, does your hospital incorporate a paper form into the hospital admissions process? How will you document in the EHR? Do you include a form on your patient portal? Do you utilize a third party to complete the process?
- In lieu of having patients complete a form, will your hospital employ an “interview based” process to obtain information and provide referrals? This patient-centric format allows for a more personal touch with attention to patient sensitivities. [6]
- Meet with the HIM Coding Manager and CDI Manager to update hospital-specific guidelines in assigning ICD-10 CM “Z codes” to all records. ICD-10-CM – “Z codes” can be assigned without provider documentation. Guidelines allow assignment of “Z codes” using any available form of documentation [7]. Develop a list of “Z codes” to be utilized based on the screening tool. Note: There is currently a joint effort initiated by UHC and AHA to expand the SDoH ICD-10 CM codes set for more SDoH specificity. [8]
Step 3: Develop a standardized workflow
Identify your next steps by developing a standardized workflow and following up with all stakeholder input:
- Identify the responsibilities of clinical teams to follow up (i.e., social workers, nurses, patient navigators, etc.) once SDOH have been captured.
- Develop a resource directory to include local partnerships (for example, food banks, meals on wheels, housing first program, shelters, community based utility grants, religious affiliations, volunteer services and so on). Assign responsibility for regular updates to this directory.
- Build community partnerships based on needs identified in the Community Needs Assessments. Community organizations can play a pivotal role in further identifying resources.
- Involve the hospital workforce and the community at large in efforts to “get the word out.”
- Hold local town hall meetings and smaller focus groups to assess community needs and brainstorm and collaborate to gain further insight to accurately reflect your community needs.
“Screening for social needs represents a major care-delivery innovation, and physicians and hospitals may need additional processes to link patients with local resources to address identified needs.” [3]
Step 4: Data Collection and sharing
- Identify the teams who will carry out vital data analysis.
- Develop your metrics. Identify how to measure success and quantitate ROI with SDOH interventions.
- Measure, refocus, and change course if necessary.
Step 5: Celebrate success and patient stories with your community and stakeholders
In moving forward with this five step SDOH readiness plan, all hospitals must carry out constant reassessment and remember that innovation is the key to the next frontier in hospital strategic planning.
Innovation is the key to the next frontier in hospital strategic planning for SDOH readiness. Click To Tweet
Addressing the social needs of patients can lead to many benefits for patients and hospitals. By implementing a SDOH Readiness Plan, innovative strategies will be identified, and solutions to individual and community problems can be addressed. This enables improved patient health, lowering costs of care, and increasing levels of trust between healthcare providers and their patients.
References
[2] https://www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-of-health
[3] Fraze TK, Brewster AL, and Lewis VA. Prevalence of Screening for Food Insecurity, Housing Instability, Utility Needs, Transportation Needs, and Interpersonal Violence by US Physician Practices and Hospitals. JAMA Netw Open. 2019;2(9):e1911514. doi:10.1001/ jamanetworkopen.2019.11514.
[4] https://www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-of-health
[8] https://www.cdc.gov/nchs/data/icd/social-determinants-of-health.pdf
[9] Mathew, J, Hodge, C, and Khau, M. Z Codes Utilization among Medicare Fee-for-Service (FFS) Beneficiaries in 2017. CMS OMH Data Highlight No. 18. Baltimore, MD: CMS Office of Minority Health. 2019.



